-
Lyme disease is a clinical diagnosis, based on a patient’s medical history, signs and symptoms and possible exposure to ticks carrying the disease.
Laboratory blood tests can be used to support a diagnosis, although current tests have low sensitivity and can miss a large number of cases.
-
-
The disease can be challenging to diagnose because the acute presentation often resembles a flu-like illness and symptoms can be nonspecific. Lyme disease symptoms can be distinguished from other illnesses, in that symptoms can change, wax and wane in severity or come and go over time. [1]
Identifying Lyme disease in children and adolescents can be especially difficult for several reasons. Young children have a limited medical history and no baseline for clinicians to compare symptoms with. Their immune system is not yet fully developed, so they’re more prone to contracting common bacterial or viral infections, characterized by flu-like symptoms – making Lyme disease easy to miss. Changes in cognition and behavior may be blamed on developmental stages. And lastly, children may struggle with describing or recognizing their symptoms when the infection has disseminated.
One study estimates that 40% of early Lyme disease cases are not diagnosed and go on to develop late Lyme disease. [2]
Bulls-eye rash
The erythema migrans (EM) rash, or bull’s-eye rash, is the tell-tale sign of Lyme disease. It is the only objective physical sign that, when present, should confirm the diagnosis of Lyme disease. The rash usually begins at or near the site of the tick bite. It usually appears within 7 to 14 days after the bite but can take up to 30 days to appear. As the infection is disseminating, rashes can appear on different parts of the body and take different forms.
Tick bites on young children frequently occur in the neck and head region. Rashes may be hidden beneath the hair on the scalp. Take extra care to check these areas on your child.
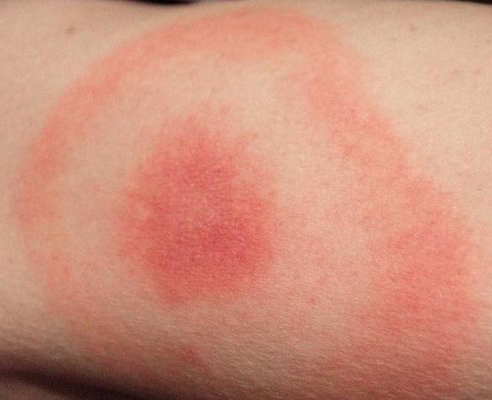 “Diagnosis of early Lyme disease is based on a physicians ability to recognize erythema migrans.” [3] A study by Johns Hopkins found that “among those with a rash, the diagnosis of erythema migrans was initially missed in 23% of patients.” [4]
“Diagnosis of early Lyme disease is based on a physicians ability to recognize erythema migrans.” [3] A study by Johns Hopkins found that “among those with a rash, the diagnosis of erythema migrans was initially missed in 23% of patients.” [4]It is widely reported that 60% to 80% of Lyme disease patients will develop the EM rash. But that figure is an overestimate and can give parents a false sense of security. The percentage of patients who present with a rash is disputed and studies vary.
For instance, studies have found that fewer than 50% of patients report an EM rash. A 2010 study conducted in Maine found that only 43% of the Lyme disease participants recalled the characteristic bull’s-eye rash. Dr. Charles Ray Jones points out that in his clinical experience, only 7% of pediatric patients report seeing the EM rash, while secondary EM rashes appear in 3% to 5% of the cases.
Take away: Don’t rely on seeing a bulls-eye rash to suspect Lyme disease.
Blood tests
Serological testing (blood tests) to identify antibodies to the Lyme bacteria can be used to help support a diagnosis. But current tests have low sensitivity and are unreliable. Patients must wait 4 to 6 weeks after the tick bite before being tested, since it takes several weeks for a person to develop enough antibodies to be detected in the blood.
The CDC recommends a two-tier process using two types of tests. The ELISA (enzyme-linked immunosorbent assay) and the Western Blot. Doctors typically order the ELISA and if positive, will order the Western Blot to confirm the diagnosis. If negative, the Western Blot is not performed. For a Lyme disease diagnosis to be made, BOTH tests must be positive.
This method has been hotly contested within the medical community, because it requires that BOTH tests are positive for a diagnosis to be made. Yet, studies indicate that both tests have low sensitivity. In fact, the ELISA has been found to miss between 35% and 50% of culture proven Lyme disease cases.
-
IGeneX Labs representative discusses Lyme disease testing.
-
Holly Ahern, Professor of Microbiology and co-founder of Lyme Action Network, explains the two-tier testing process for Lyme disease.
-
References
[1] National Institutes of Allergy and Infectious Diseases (NAID)
www.niaid.nih.gov/topics/lymedisease/understanding/pages/intro.aspx[2-3] John Hopkins School of Public Health
www.jhsph.edu/research/centers-and-institutes/mid-atlantic-public-health-training-center/_documents/051513_Lyme_Disease_Aucott.pdf[4] BMC Infectious Diseases
www.biomedcentral.com/1471-2334/9/79



